5 Reasons Your African Healthcare Facility Needs a Hospital Management System Now
Adopting a Hospital Management System (HMS) is no longer a luxury but a necessity for African healthcare facilities aiming to improve patient outcomes, operational efficiency, and financial sustainability.
Given the unique challenges of the region, including high patient volumes, limited resources, and the need for better data management, a digital transformation is essential to stay competitive and provide quality care.
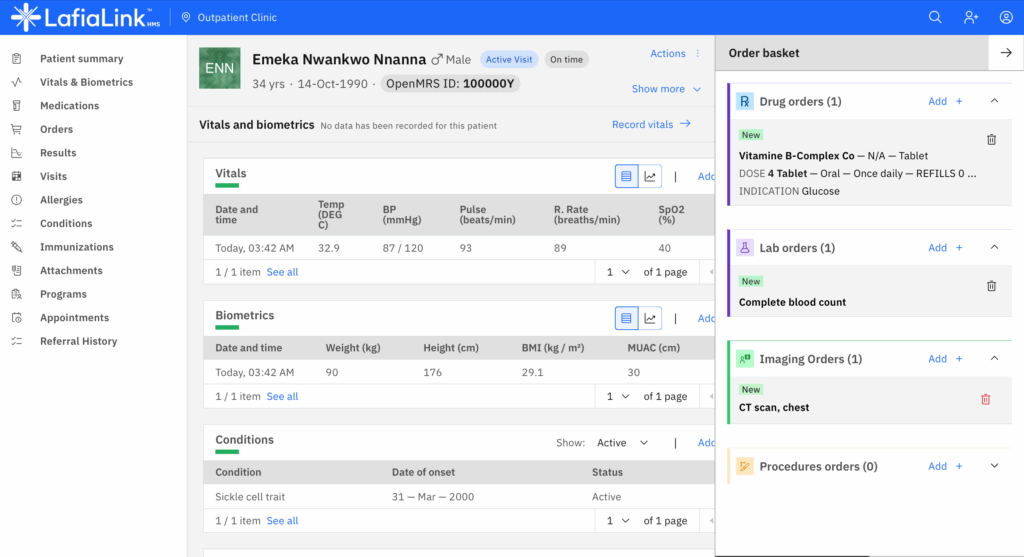
Yet, despite these pressures, many hospitals and clinics continue to rely on paper-based systems and manual processes that drain resources, compromise patient safety, and hinder operational efficiency.
The adoption of Hospital Management Systems (HMS)—also known as Hospital Information Systems (HIS) or Electronic Health Records (EHR)—represents not merely a technological upgrade, but a fundamental transformation in how healthcare is delivered, managed, and experienced across Africa.
Research indicates that EHR adoption among healthcare professionals in Africa remains suboptimal, with studies showing that merely 27.3% of nurses indicate proficient engagement with electronic systems, and 80.1% of nurses in some Nigerian teaching hospitals report never using available digital systems despite infrastructure being in place .
However, the trajectory is changing. The COVID-19 pandemic accelerated digital transformation, mobile penetration continues to rise exponentially, and there’s growing recognition that technology-enabled healthcare is essential for achieving Universal Health Coverage (UHC) goals.
This article presents five evidence-based reasons why implementing a Hospital Management System is no longer optional but essential for healthcare facilities across Africa—from bustling urban tertiary hospitals to rural primary care clinics.
1. Eliminating Dangerous Medical Errors and Enhancing Patient Safety
The Cost of Paper-Based Systems
In healthcare, errors cost lives. Across African facilities relying on paper records, the risks are manifold: illegible handwriting, misplaced files, incomplete patient histories, and medication errors due to lack of access to allergy information or previous prescriptions.
A study examining nursing documentation in Nigerian hospitals found that quality was “predominantly poor” in electronic wards before proper system implementation, with 85.1% of documentation rated as poor quality initially.

However, following structured electronic system implementation with standardized care plans, poor documentation declined significantly to 20.6%, demonstrating the potential for dramatic improvement.
How HMS Transforms Patient Safety
A comprehensive Hospital Management System creates a centralized, accessible repository of patient information that follows the patient throughout their healthcare journey.
When a patient arrives at your facility, clinicians can immediately access complete medical histories, including previous diagnoses, allergies, current medications, and treatment responses.
This longitudinal tracking is particularly critical as Africa undergoes an epidemiological transition, shifting from infectious diseases to chronic conditions like diabetes, hypertension, and cardiovascular diseases that require consistent, long-term management .
Real-World Impact:
Medication Safety: Electronic prescribing eliminates errors from illegible handwriting and enables automatic checks for drug interactions, allergies, and contraindications
Clinical Decision Support: Systems like the electronic Integrated Management of Childhood Illness (eIMCI) implemented in South African primary care clinics provide practitioners with protocol guidance, improving adherence to evidence-based care standards
Reduced Duplicate Testing: With instant access to previous laboratory results and imaging studies, unnecessary repeat tests are eliminated, reducing costs and patient inconvenience while preventing treatment delays
Addressing Africa-Specific Safety Challenges
In resource-constrained settings, HMS addresses unique safety concerns. Power failures and technical disruptions, common in many African regions, can be mitigated through robust HMS design with offline capabilities and backup systems.
Research from South Africa emphasizes that while technical disruptions occur, regular system evaluations and compliance with standards like NIST cybersecurity frameworks ensure resilience .
Furthermore, standardized digital tools reduce variability in care quality between urban tertiary centers and rural clinics, addressing the urban-rural healthcare divide that characterizes many African health systems.
2. Dramatically Improving Operational Efficiency and Resource Utilization
The Efficiency Crisis in African Healthcare
Healthcare facilities across Africa operate under severe resource constraints—financial, human, and infrastructural. Yet, studies reveal that paper-based administrative processes consume disproportionate amounts of valuable staff time.
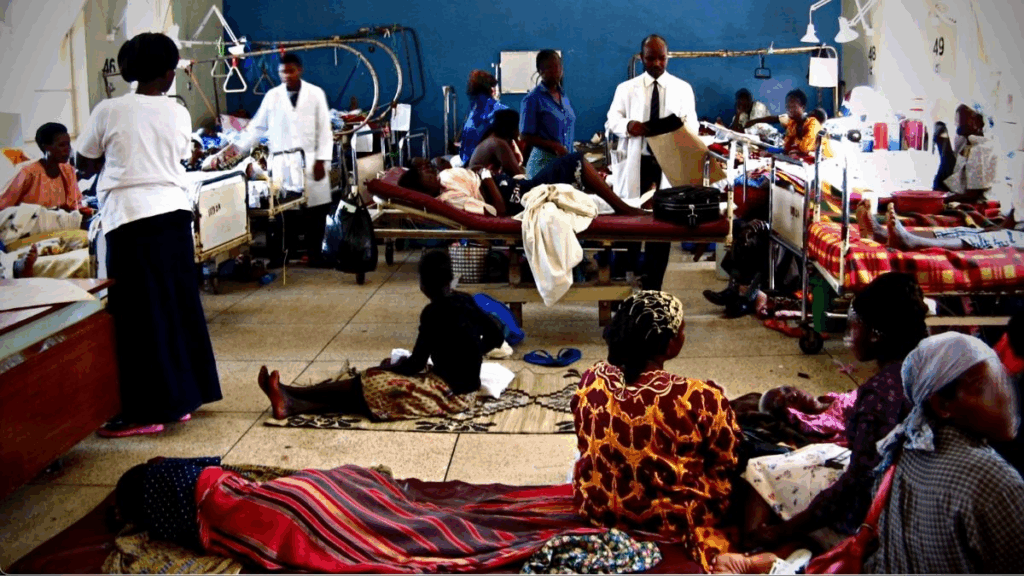
Research from South African community health centers found that reliance on paper-based records resulted in “increased workloads and errors,” with nurses recognizing obstacles including “data redundancy, misfiling, absence of a chronological patient timeline, excessive documentation time, and diminished patient care opportunities” .
Streamlining Operations Through Digital Transformation
A Hospital Management System integrates all core operational functions, patient registration, appointment scheduling, billing, inventory management, laboratory workflows, pharmacy dispensing, and clinical documentation—into a unified platform.

This integration eliminates silos, reduces duplication, and enables seamless information flow across departments.
Key Efficiency Gains:
Administrative Automation: Routine tasks such as patient registration, insurance verification, and billing calculations are automated, reducing waiting times and freeing staff for patient-facing activities. Research demonstrates that efficient billing and financial management significantly reduce patient waiting times, contributing to a more positive healthcare experience .
Inventory and Supply Chain Management: For African facilities struggling with stockouts of essential medicines and supplies, HMS inventory modules provide real-time tracking, automated reorder alerts, and consumption analytics. This prevents both shortages that compromise care and overstocking that ties up limited capital.
Resource Optimization: Bed management modules enable real-time visibility of bed occupancy, streamlining admissions and transfers. Operating theater scheduling modules maximize utilization of expensive surgical facilities. Staff scheduling tools ensure optimal deployment of scarce human resources based on patient volumes and acuity.
Financial Sustainability
Efficiency translates directly to financial sustainability. By reducing administrative overhead, minimizing waste, and optimizing resource utilization, HMS enables facilities to serve more patients with existing resources.
For private facilities, faster billing cycles and reduced revenue leakage improve cash flow. For public facilities, efficiency gains mean stretched government budgets deliver more healthcare services to populations in need.
3. Enabling Data-Driven Decision Making and Quality Improvement
The Current Data Vacuum
In many African healthcare facilities, strategic decision-making occurs in a data vacuum. Managers lack accurate, timely information about service utilization, disease patterns, treatment outcomes, or operational performance.
Aggregating data from paper records is labor-intensive, error-prone, and inevitably retrospective—decisions are based on months-old information that fails to reflect current realities.
Transforming Data into Intelligence
A Hospital Management System automatically captures structured data at every patient touchpoint, creating a foundation for real-time analytics and evidence-based management.
Clinical Intelligence:
Disease surveillance and outbreak detection through automated reporting of notifiable conditions
Treatment outcome tracking for quality improvement initiatives
Population health analytics identifying high-risk patient groups requiring targeted interventions
Clinical audit capabilities supporting continuous professional development and accreditation requirements
Operational Intelligence:
Real-time dashboards showing patient volumes, waiting times, and service utilization patterns
Financial analytics tracking revenue, costs, and profitability by service line
Staff productivity metrics supporting performance management and resource allocation
Predictive analytics forecasting patient demand and resource requirements
Supporting National Health Information Systems
Individual facility HMS implementations contribute to broader health system strengthening. As research from South Africa emphasizes, cloud and data analytics capabilities enable aggregation of facility-level data for district, provincial, and national health information systems, critical for policy formulation, resource allocation, and monitoring progress toward health targets like the Sustainable Development Goals .
However, this requires attention to data standardization, interoperability, and compliance with national health information architecture standards.
4. Enhancing Accessibility and Continuity of Care Across the Care Continuum
The Fragmentation Challenge
African healthcare delivery is often fragmented, with patients moving between public and private sectors, primary care and referral hospitals, and traditional and modern medicine practitioners.
Without information continuity, each encounter starts anew—clinical decisions are made without context, previous investigations are repeated, and care plans are disjointed.
This fragmentation is particularly harmful for patients with chronic conditions requiring long-term management.
Creating Connected Care Networks
Hospital Management Systems, particularly when implemented with interoperability standards, enable seamless information sharing across the care continuum.
Referral Coordination: When a primary care clinic refers a patient to a tertiary hospital, complete clinical information, including investigation results, treatment history, and referral reasons, transfers electronically.
This eliminates the common scenario of patients arriving at referral centers with nothing but a paper referral letter, forcing clinicians to reconstruct histories from patient memory.
Continuity Across Encounters: Whether a patient visits your facility today, next month, or next year, their complete record is instantly accessible. This is particularly valuable for managing chronic diseases, antenatal care, pediatric growth monitoring, and HIV/AIDS treatment programs where longitudinal tracking is essential.
Telemedicine Integration: The COVID-19 pandemic accelerated telemedicine adoption across Africa, addressing access barriers for rural populations and reducing unnecessary travel. HMS platforms that integrate telemedicine capabilities enable remote consultations while maintaining comprehensive documentation within the patient record.
However, research notes challenges including limited broadband access in rural areas and the need for regulatory frameworks governing telemedicine practice .
Mobile Health (mHealth) Synergies
Africa leads the world in mobile health innovation. HMS integration with mHealth applications enables patient engagement through appointment reminders, medication adherence support, and health education.
For facilities, mobile interfaces extend system access beyond desktop computers, enabling point-of-care documentation using tablets or smartphones—critical in settings with limited computer availability.
5. Strengthening Financial Management and Sustainability
Revenue Leakage and Inefficiency
Financial sustainability remains a critical challenge for African healthcare facilities. Paper-based billing systems are prone to errors, omissions, and fraud—services are provided but not charged, charges are miscalculated, and revenue slips through administrative cracks.
For cash-strapped public facilities, this represents lost resources that could fund additional staff, medicines, or equipment. For private facilities, it threatens viability and return on investment.
Financial Management Capabilities
Modern Hospital Management Systems include comprehensive financial modules that transform revenue cycle management:
Automated Billing: Integration with clinical modules ensures all services, consultations, procedures, medications, supplies, and investigations, are automatically captured and billed accurately.
This eliminates the common scenario where busy clinicians provide care but fail to document chargeable services.
Insurance and NHIS Integration: In countries with National Health Insurance Schemes (NHIS) or robust private insurance markets, HMS integration with payer systems enables real-time eligibility verification, claims submission, and payment tracking.
This reduces claim rejections, accelerates reimbursement, and improves cash flow.
Cost Accounting: Activity-based costing modules enable facilities to understand true costs of service delivery, informing pricing decisions and identifying opportunities for efficiency gains.
This is essential for facilities operating in competitive markets or participating in results-based financing schemes.
Transparency and Accountability: Digital financial systems create audit trails that deter fraud and corruption, significant concerns in many African health systems. Automated reconciliation between clinical activity and financial records ensures accountability.
Return on Investment
While HMS implementation requires upfront investment, research demonstrates compelling returns. Efficiency gains reduce operational costs, revenue capture improvements increase income, and quality enhancements attract more patients.
For African facilities, cloud-based HMS solutions reduce infrastructure requirements, while open-source options like OpenMRS (originally developed for HIV care in Kenya and Rwanda) lower licensing costs.
The key is selecting solutions appropriate to local contexts—avoiding over-engineered systems that create complexity without commensurate benefit .
Implementation Considerations for African Contexts
Addressing Adoption Barriers
Research consistently identifies key barriers to HMS adoption in Africa: insufficient training, limited computer literacy among healthcare workers, workflow disruptions during transition, connectivity issues, and resistance to change . Successful implementation requires:
Comprehensive Change Management: Technology implementation is fundamentally about people. Facilities must invest in training programs that build digital literacy alongside system-specific skills.
Studies show that targeted computer skill training significantly improves adoption rates, while usability optimization is crucial for boosting confidence .
Infrastructure Resilience: Given power and connectivity challenges, HMS selection must prioritize offline functionality, backup systems, and low-bandwidth operation. Cloud solutions with local caching capabilities offer advantages over purely web-based systems.
Contextual Appropriateness: Systems must align with local workflows, regulatory requirements, and language needs. Attempting to implement complex, foreign-designed systems without adaptation creates frustration and abandonment.
Research from Nigeria found that perceived usefulness—how well the system fits local needs—was the strongest predictor of adoption intention, with an odds ratio of 18.357 .
Phased Implementation: Rather than big-bang deployments that disrupt operations, successful facilities implement modules sequentially—starting with patient registration and billing before expanding to clinical documentation and advanced analytics.
Regulatory and Security Considerations
As African countries strengthen data protection frameworks—such as South Africa’s Protection of Personal Information Act (POPIA)—HMS implementation must prioritize security and compliance.
This includes access controls, audit logging, encryption, and data residency considerations when using cloud solutions. Research emphasizes the importance of regular security assessments and compliance with international standards like ISO 27000 series and NIST frameworks .
The evidence is clear: Hospital Management Systems are not luxury technologies for wealthy healthcare systems but essential tools for African facilities striving to deliver quality, efficient, sustainable care.
From eliminating dangerous medical errors and improving operational efficiency to enabling data-driven management and ensuring financial viability, HMS addresses the core challenges facing African healthcare today.
The adoption statistics, while currently showing room for improvement—are trending upward as more facilities recognize the competitive and clinical necessity of digital transformation.
With appropriate implementation strategies that address local context, infrastructure constraints, and human factors, African healthcare facilities can leapfrog the problematic implementations seen elsewhere and realize the full potential of health information technology.
For healthcare leaders across the continent, the question is no longer whether to implement a Hospital Management System, but how to do so effectively, sustainably, and in ways that truly serve the needs of African patients and communities.
The investment in HMS is an investment in better health outcomes, operational excellence, and the future of healthcare delivery across Africa.
References:
: Adoption of electronic health records by nurses in Africa – PMC, 2024. https://pmc.ncbi.nlm.nih.gov/articles/PMC12437165/
: Adoption of electronic medical records in developing countries—A multi-state study of the Nigerian healthcare system, Frontiers in Digital Health, 2022. https://www.frontiersin.org/journals/digital-health/articles/10.3389/fdgth.2022.1017231/full
: Challenges and Risks of Digitalizing Health Systems, ACM Digital Library, 2025. https://dl.acm.org/doi/10.1145/3759023.3759121
: 3 Ways Africa Can Avoid America’s Electronic Health Record Woes, ICT Works, 2022. https://www.ictworks.org/africa-electronic-health-record-woes/
: Digital Health Systems in Africa, IQVIA White Paper. https://www.iqvia.com/-/media/iqvia/pdfs/mea/white-paper/iqvia-digital-health-system-maturity-in-africa.pdf
: MediSys: Streamlined Hospital Management Software for Africa, CureSure Medico, 2024. https://www.curesuremedico.com/blog/medisys-revolutionizing-healthcare-management-cutting-edge-software-solutions